Maternal Mental Health Awareness Month: Why 1 in 5 Isn’t the Whole Story (Understanding Matrescence and Motherhood)
Matrescence, Motherhood and Maternal Mental Health
First and foremost - this blog is NOT clinical advice nor is it intended to minimize PMADS or maternal mental health. In fact, it is to strengthen this conversation, expand it and bring more attention to it, from all disciplines and providers who work with Mothers.
I Wasn’t the 1 in 5—But I Was Part of the 5 in 5
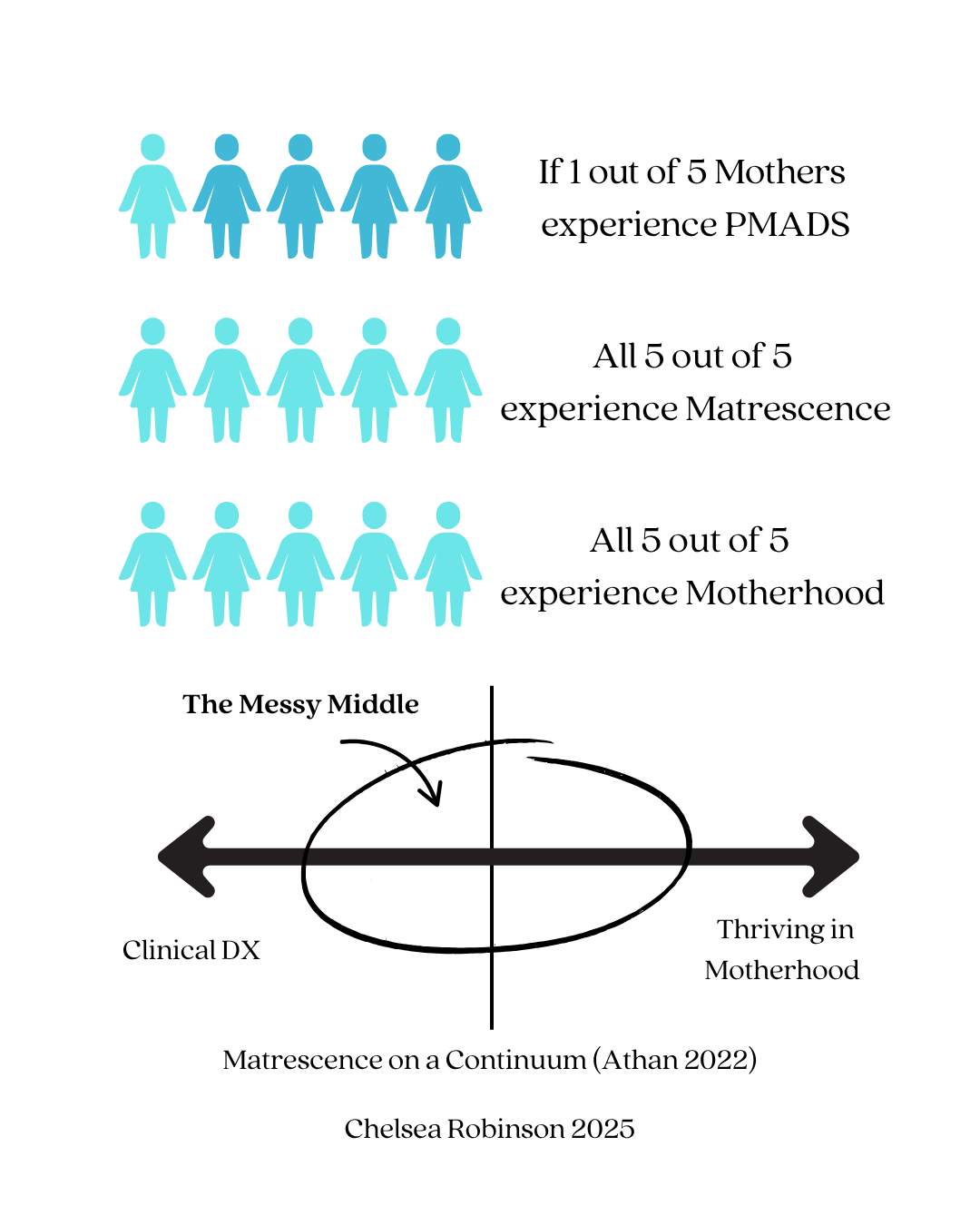
Every May, during Maternal Mental Health Awareness Month, we return to an important and necessary statistic: 1 in 5 mothers will experience a Perinatal Mood or Anxiety Disorder (PMAD).
This statistic has transformed the field of maternal mental health. It has helped name suffering that for far too long went unseen, misdiagnosed, or dismissed. It has created pathways to care and increased access to treatment for mothers who need it.
And still, there is something missing.
Because while 1 in 5 mothers will experience a diagnosable maternal mental health condition, 5 in 5 will experience Matrescence—the developmental push of becoming (and being) a mother.
That distinction is not just conceptual. It is clinically relevant, and it shapes how mothers understand themselves every day.
“In my expanded definition, the process of becoming a mother or matrescence, the term first coined by Dana Raphael, Ph.D. (1973) and which I later built further upon, is a developmental passage where a woman transitions through pre-conception, pregnancy and birth, surrogacy or adoption, to the postnatal period and beyond. The exact length of matrescence is individual, recurs with each child, and may arguably last a lifetime! The scope of the changes encompasses multiple domains— biological, emotional, social, political, spiritual— and can be likened to the developmental push of adolescence. These transformations unfold in both “brain and mind”: the maternal brain undergoes measurable morphological and functional reorganization, while the mother’s inner world undergoes profound psychological and ideological restructuring—reshaping her identity, beliefs, values, priorities, and sense of meaning or purpose.”
- Definition written by Aurélie Athan, Ph.D. (2016, updated 2026)
When You’re Not Diagnosed, But You’re Still Struggling
I wasn’t the 1 in 5.
I didn’t meet criteria for postpartum depression or anxiety. There was no diagnosis, no treatment plan, no clear clinical pathway that reflected what I was experiencing.
But something was happening.
Internally, I felt a shift I couldn’t quite name. My sense of self felt less stable. My relationships felt different. My emotional world felt more intense and exposed. It was subtle enough to fall outside diagnostic thresholds, but significant enough that it could not be ignored.
I remember trying to articulate this in therapy and slowly realizing that there wasn’t language for it in the room.
There was care but there wasn’t a framework.
And without a framework, the experience became personal. It felt like something about me wasn’t working the way it should.
Finding the Language: Understanding Matrescence
So I went looking for answers.
That search led me to Matrescence, and to the work of Aurelie Athan and Alexandra Sacks. For the first time, my experience could be understood not as individual pathology, but as part of a developmental process.
Matrescence describes the transition into motherhood as a period of profound psychological, relational, and identity reorganization similar in magnitude to adolescence. It is a universal experience, even though it unfolds differently for each mother.
That language mattered.
It shifted the question from “What is wrong with me?” to “What is happening to me?”
And yet, for me, even that didn’t fully capture it.
Matrescence Explains the Transition—But Not the Entire Context
While matrescence helped me understand the internal changes, it didn’t fully explain why the experience felt as heavy and disorienting as it did.
It didn’t account for the conditions I was mothering within.
The isolation of modern motherhood.
The invisible labor that often goes unrecognized.
The cultural expectations around what a “good mother” should be.
The relational dynamics that shift without being named or supported.
Matrescence named the transition. But it didn’t fully name the context shaping that transition.
And that gap matters, especially in how we understand maternal mental health.
Why Maternal Mental Health Is More Than Diagnosis
Maternal Mental Health Awareness Month has been essential in highlighting PMADs. These conditions are real, serious, and require timely, evidence-based care.
But when maternal mental health is understood only through a diagnostic lens, we risk narrowing our understanding of maternal experience.
Not all distress meets criteria for a disorder, but that does not mean it is insignificant.
Without a broader framework, many mothers are left without language for what they are experiencing. Developmental changes—intense, disorienting, and real—can be misinterpreted as personal inadequacy rather than understood within the context of Matrescence, identity shifts, and sociocultural pressures.
This is where misinterpretation happens. And where unnecessary self-blame can take hold.
A Both/And Approach to Maternal Mental Health
Expanding the conversation is not about minimizing PMADs. It is about holding a more complete picture.
We need a both/and framework for maternal mental health:
1 in 5 mothers experience PMADs and require clinical care
5 in 5 mothers experience matrescence and require understanding, context, and support
5 in 5 mothers experience becoming and being a Mother within Motherhood: the social, cultural, historical, economic, political context that is Motherhood today
These truths are not in competition with each other, rather they are interconnected.
Supporting maternal mental health effectively means integrating:
Clinical diagnosis and treatment
Developmental understanding
Relational awareness
Sociocultural context
When these lenses come together, care becomes more complete.
From Personal Experience to Professional Practice
This is why this has become my work. I have seen how often this gap persists; not because professionals lack skill or commitment, but because the frameworks we are trained in do not fully account for the complexity of maternal experience.
Many clinicians are equipped to identify and treat symptoms, but have had limited exposure to frameworks like matrescence, or to the ways identity, relationships, and systems shape maternal wellbeing and development.
As a result, mothers may leave sessions with strategies but without a deeper sense of understanding.
And understanding matters because when a mother can locate her experience within a broader developmental and contextual framework, something shifts. The narrative moves from “something is wrong with me” to “something is happening to me.”
That shift can make all the difference between pathology and normative development.
Reframing Maternal Mental Health
Maternal mental health does not exist outside of maternal development; in fact, it is shaped by it.
When we expand our lens in this way:
Distress can be understood within context, not immediately pathologized
Identity disruption can be recognized as part of development
Relational and systemic factors move to the center of care
Mothers are met with clarity, not just coping strategies
This is about expanding the conversation on maternal mental health; not minimizing distress or pathology.
Moving Forward During Maternal Mental Health Awareness Month
As Maternal Mental Health Awareness Month continues to grow, the opportunity before us is not only to raise awareness but to deepen and expand our understanding.
To move beyond an either/or framework and toward a more integrated model of care that reflects the full reality of maternal experience.
Because being outside the 1 in 5 does not necessarily mean a mother is okay, nor should it assume she is suffering.
Being part of the 5 in 5 means she deserves language, context, and support too.
Interested in reading more? I recently contributed to Jessie Harrold’s collection “Mother Becoming: Reflections and Scholarship on Matrescence” and you can read my piece “Differentiating Between PMADs and Matrescence: A Critical Examination of Maternal Development and Its Pathological Interpretations” available for purchase here.
Learn More and Get Involved
Professionally: The Matricentric Way is leading this paradigm shift - it truly is expanding the conversation on maternal mental health. If you are a professional that supports Mothers, I invite you to enroll in The Matricentric Way, either LIVE or self-paced. Join this movement today so that we can transform not only the lives of the individual Mothers we support, but the greater collective of Mothers.
Additionally, Matrescence, Motherhood and Maternal Mental Health Clinical Consultation is offered monthly for therapists seeking to expand their understanding of this unique intersection. Learn more here.
Personally: The Becoming Mama course is available self-paced for any Mother within her first 7 or so years postpartum, interested in learning more about her matrescence AND the impact of Patriarchal Motherhood on her experience of being a Mother. (NOTE: this is NOT a substitute for clinical therapy NOR is it recommended to treat maternal mental health challenges. Consult your therapist for any mental health concerns.)
Download the CARE Model – Start the shift with our free introduction guide to dismantling the mental load and re-imagining care.
Purchase The CARE and HOLD Model for Professionals here. And if you are interested in this model personally, you can purchase the Guide here.